Baritastic Surgery
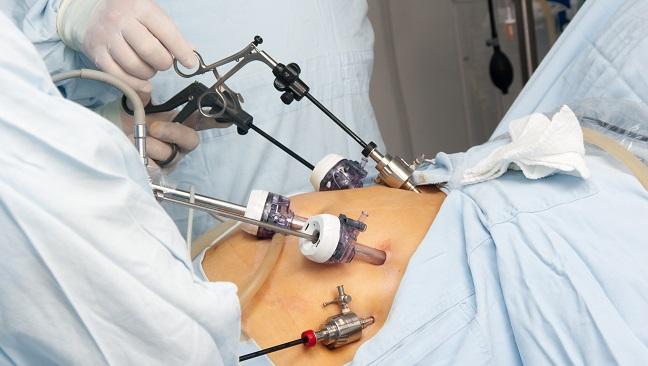
Bariatric surgery (weight loss surgery) includes a variety of procedures performed on people who have obesity. Weight loss is achieved by reducing the size of the stomach with a gastric band or through removal of a portion of the stomach (sleeve gastrectomy or biliopancreatic diversion with duodenal switch) or by resecting and re-routing the small intestine to a small stomach pouch (gastric bypass surgery).
Long-term studies show the procedures cause significant long-term loss of weight, recovery from diabetes, improvement in cardiovascular risk factors, and a mortality reduction from 40% to 23%. Bariatric surgery for obese people with a body mass index (BMI) of at least 40, and for people with BMI of at least 35 and serious coexisting medical conditions such as diabetes. However, research is emerging that suggests bariatric surgery could be appropriate for those with a BMI of 35 to 40 with no comorbidities or a BMI of 30 to 35 with significant comorbidities. Metabolic & Bariatric Surgery guidelines suggest the position statement on consensus for BMI as an indication for bariatric surgery. Bariatric surgical procedures cause weight loss by restricting the amount of food the stomach can hold, causing malabsorption of nutrients, or by a combination of both gastric restriction and malabsorption. Bariatric procedures also often cause hormonal changes.
Recommended: - Diabetes conferences | Obesity conferences | Endocrinology conferences | Diabetes2023 | World congress on diabetes | Diabetes meetings | Endocrinology meetings | World diabetes congress |